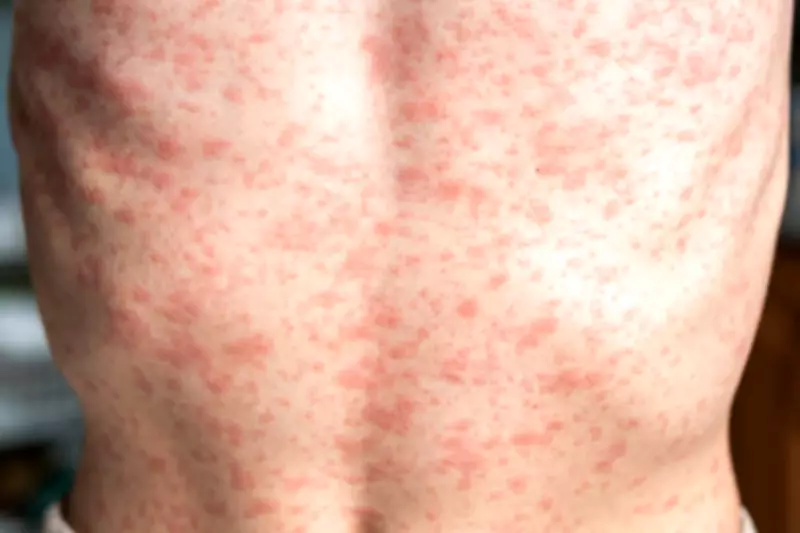
Measles Outbreak Intensifies in Utah with 602 Confirmed Cases
The measles virus, which resides in the nose and throat mucus of infected individuals, has triggered a significant outbreak in Utah, with state officials confirming 602 cases as of April 2026. Alarmingly, 85% of those infected had not received the measles vaccine, highlighting a critical gap in immunization coverage. This outbreak represents the latest in a series of measles surges across the United States since early 2025, with additional clusters reported in Texas, New Mexico, and Oklahoma.
National Measles Cases Reach Highest Level Since 1991
According to the Centers for Disease Control and Prevention (CDC), the United States recorded 2,287 confirmed measles cases in 2025, marking the highest number since 1991. Dr. Lisa M. Lee, a research professor of population health sciences at Virginia Polytechnic Institute and State University, attributes this trend to insufficient vaccination rates. "The primary driver behind the 19 measles outbreaks so far in 2026 is the same one that drove the 48 outbreaks last year – too few people vaccinated to reach herd immunity," she explains. Communities require at least a 95% vaccination rate to effectively contain measles, given its extreme contagiousness.
Historical Context and Elimination Status at Risk
Measles was officially eliminated in the United States in 2000, following rigorous reviews by the CDC, an external expert panel, and the Pan American Health Organization. However, the recent surge in cases threatens this status. The last major outbreak before 2025 occurred in 2019, involving nearly 1,300 cases, which nearly jeopardized the nation's elimination standing. Dr. Peter Hotez, dean of the National School of Tropical Medicine at Baylor College of Medicine, notes that declining vaccination rates both domestically and globally have contributed to a fourfold increase in measles outbreaks from 2023 to 2024.
Understanding Measles: Transmission and Symptoms
Measles is a respiratory virus primarily affecting children, though unvaccinated adults are also susceptible. The virus spreads through airborne particles when infected individuals cough, sneeze, or breathe, with these particles remaining infectious in the air for up to two hours. Direct contact is not necessary for transmission, making measles one of the most contagious viruses known. The CDC estimates that if one person has measles, up to 90% of unvaccinated individuals exposed to contaminated air or surfaces will contract the virus.
Symptoms typically appear one to two weeks after exposure and include:
- Cough, runny nose, and red, watery eyes
- High fever
- Tiny white spots inside the mouth (Koplik's spots)
- A red rash that starts on the face and spreads to the body
Infected individuals are contagious for about eight days, including four days before the rash appears, which complicates containment efforts.
Complications and High-Risk Groups
While most people recover from measles without long-term effects, complications can be severe. According to the CDC:
- One in 10 children develops ear infections
- Up to one in 20 contracts pneumonia, the leading cause of measles-related deaths in young children
- One in 1,000 experiences encephalitis (brain swelling), which can lead to deafness, convulsions, or intellectual disability
- One to three in 1,000 children die from these complications
Unvaccinated individuals, children under five, adults over 20, immunocompromised people, and pregnant women face the highest risks. There are no specific treatments for measles, though vitamin A may reduce severity in some hospitalized patients.
Prevention Through Vaccination
Vaccination remains the most effective prevention strategy. The measles, mumps, and rubella (MMR) vaccine is administered in two doses: the first at 12-15 months (93% effective) and the second at 4-6 years (97% effective). Before the U.S. vaccination program began in 1963, measles caused 3-4 million cases annually, with thousands of hospitalizations and hundreds of deaths.
The vaccine is safe, with extensive research debunking a fraudulent 1998 study linking it to autism. For those exposed to measles, post-exposure vaccination within 72 hours or immunoglobulin treatment within six days can mitigate infection risks. Vaccination and natural infection both confer lifelong immunity.
Current Concerns and Herd Immunity Challenges
The CDC expresses concern over measles in the U.S., citing declining vaccination rates fueled by anti-vaccine rhetoric. From the 2019-20 to 2024-25 school years, kindergarten vaccination rates dropped from 95% to 92.5%, below the 95% threshold needed for herd immunity. States like Idaho have rates as low as 78.6%. Dr. Robert Bednarczyck, an epidemiologist at Emory University, warns, "We're potentially sitting right on the edge of where we might start seeing more widespread outbreaks." Experts emphasize that maintaining high vaccination coverage is crucial to preventing future epidemics and protecting vulnerable populations.









